BIOLOGICAL AND HEALTH SCIENCES
Scientific experiment leads to bone regeneration
CONICET researchers applied a gel that promotes bone reconstruction in one animal injury model and it was a success.
In Rosario a research team led by Sara Feldman, CONICET independent researcher, participated in a multidisplinary tissue engineering study. These scientists developed a biodegradable gel that promotes bone regeneration and applied it on an in vivo model, that is to say, in living beings. Thus, traditional prosthesis of some type of injuries can be replaced.
This study was published in Tissue Engineering and was conducted with researchers who belong to different institutions such as: the Instituto Bioforge (Universidad de Valladolid, España); the Planta Piloto de Procesos Industriales Microbiológicos (PROIMI) under the scope of the CONICET; and the Universidade de Ribeirão Preto, Brazil.
The researchers applied biodegradable gel on an experimental injury model of rabbits. After 90 days, they proved that that material had promoted the development of a tissue that has a formation and appearance similar to the original bone structure in the injury location.
The gel was synthesized through molecular biology techniques and some of its components are natural elastin derivatives, sequences for cell adhesion proteins and one protein called BMP-2 that promotes bone development.
One striking characteristic of this gel is that contrary to the most well-known gelatins, it is in liquid state under low temperatures and “gelifies” when it exceeds the four degree centigrade. This characteristic made the Laboratorio de Biología Osteoarticular, Ingeniería Tisular y Terapias Emergentes (Laboatem) develop special surgical techniques to apply the gel.
“Apart from the necessary sterile conditions for a surgery, we had to work everything in cold, even the equipment, to maintain the matrix in a liquid state to put it on the injury and make it gelify with the temperature of the body”, the researcher, who leads the Laboatem at the la Facultad de Ciencias Médicas de la Universidad Nacional de Rosario, describes.
The scientists had tested the biodegradable material in some kind of femoral injury. If an implant is not put there, a structural and functional fibrous tissue that is different from the original grows on the injury. With the application of the gel, some days after the surgery, the rabbits had already begun to move as they normally do, which means that there were neither inflammatory processes nor rejections. The studies were complemented with biochemical analysis throughout the research and there were not altered parameters observed.
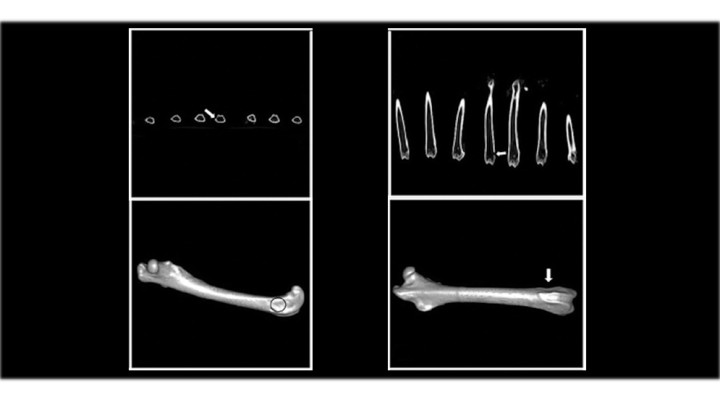
“We conducted the tomographic studies with tridimensional bone reconstruction and observed that the injuries were fixed, with a cortical surface almost regenerated. At first sight it was difficult to distinguish the place of the implant. Through the histological studies, we also found areas of calcification and osteoblasts, a pattern of bone tissue”, Feldman describes.
Once the material is inserted in the injury, the gel promotes the cell proliferation that surrounds it so these cells colonize the tissue and form an extracellular matrix similar to the bone. As the material plays its role, it breaks down and disappears at the end of the process.
For Feldman, this type of gels are third-generation matrixes. The first-generation ones, are the bone implants; the second-generation ones are the metallic prosthesis that receive different types of treatments to avoid the rejection of the body, and the matrixes derived from natural products. The third-generation matrixes are the ones that are temporary, biodegradable, non-toxic for cells, and pretend to regenerate the tissue under the most common conditions for the original missing tissue.
“With these tests, we managed to analyze the viability of this third-generation matrix on an in vivo model that is different from the in vitro –cells in culture– analysis because we can observe if there are side effects, if it adapts to the surrounding tissue or if there is some kind of immune rejection”, Feldman explains. He concludes that “this type of studies show the bone engineering is not a utopia, it can contribute to fix injuries in vivo.”
By Vanesa Bomben
CONICET Rosario
Research team
Laboatem
Dante Coletta
Ezequiel Vitelli
Mariangeles Aimone
Facundo Zabalza
Sara Feldman
Universidad Nacional de Tucumán
Liliana Missana
María Jammal
Universidad de Valladolid
Arturo Ibáñez-Fonseca
Matilde Alonso
José Carlos Rodríguez-Cabello
Universidad de San Pablo
João Paulo Mardegan Issa